Let me guess—you’ve tried the meditation apps, cleaned up your diet, maybe even dipped into therapy.
But the anxiety still rolls in like a storm front.
Your chest tightens for no reason.
Your heart is pounding like you ran a marathon and you can’t catch your breath.
Your sleep is trash.
And despite all your efforts, you still feel like you’re one “urgent” email away from a full-on internal meltdown.
Here’s what no one told you: your anxiety might not start in your head—it might start in your gut. This is what scientists call the gut-brain connection.
Those ambiguous symptoms that confuse your doctors – like chronic digestive issues, brain fog, sleep problems, and that familiar undercurrent of panic or doom – are easy to blame on stress, personality, maybe even past trauma.
But what if you have a raging case of leaky gut, sky-high histamine levels, and gut bacteria making neurotoxins that are basically giving your brain the middle finger?
You’re not alone.
The science is clear: your gut and brain are in constant communication (4, 18, 25).
When the gut is inflamed, leaky, or overrun with microbial chaos, the brain feels it.
It reacts.
Let’s unpack how healing your gut can bring you peace of mind—literally.
Key Takeaways
- Anxiety often starts in the gut—not the head.
- Hidden gut disruptors—like histamine, mold, parasites, and EMFs—can mimic or trigger anxiety.
- You can’t supplement your way out of this, but it is fixable!

Gut and Brain Health: A Preview of What’s to Come
There are So. Many. Ways in which your gut is associated with anxiety. Here are some of them:
- Inflammation (8, 13, 19, 21, 24)
- Dysbiosis (9, 13, 24, 25)
- Microbiome impacts HPA axis and influences anxiety (4, 18)
- Intestinal permeability (4, 8, 17)
- Histamine receptor activation (22)
- Decreased neurotransmitters, brain derived neurotrophic factor, and short-chain fatty acids such as butyrate (4, 7, 8, 18, 20, 24, 25)
- Oxidative stress (8, 11)
- Constipation (16)
- Visceral pain (1, 7)
- Bile acid alterations (8, 12)
More on some of these later.
Additionally, there are several exposures you may have that can trigger intestinal chaos or neuroinflammation, leading to anxiety (that’s why a root cause assessment is critical).
- Parasitic infections (6, 7, 17)
- Mold exposure (28, 29)
- Poor diet / ultra processed foods (8, 14)
- Exposure to chemicals such as BPA (5)
- Exposure to herbicides and pesticides such as glyphosate and atrazine (30, 31)
- Heavy metals (mercury, lead, aluminum, cadmium, etc.) (32, 33)
- EMF’s that can increase mast cell, parasite, and mold activity (34, 35, 36)
Many of these have been discussed in other blogs, so if you’re curious, be sure to check them out. For now, let’s review how the gut and brain communicate with each other.
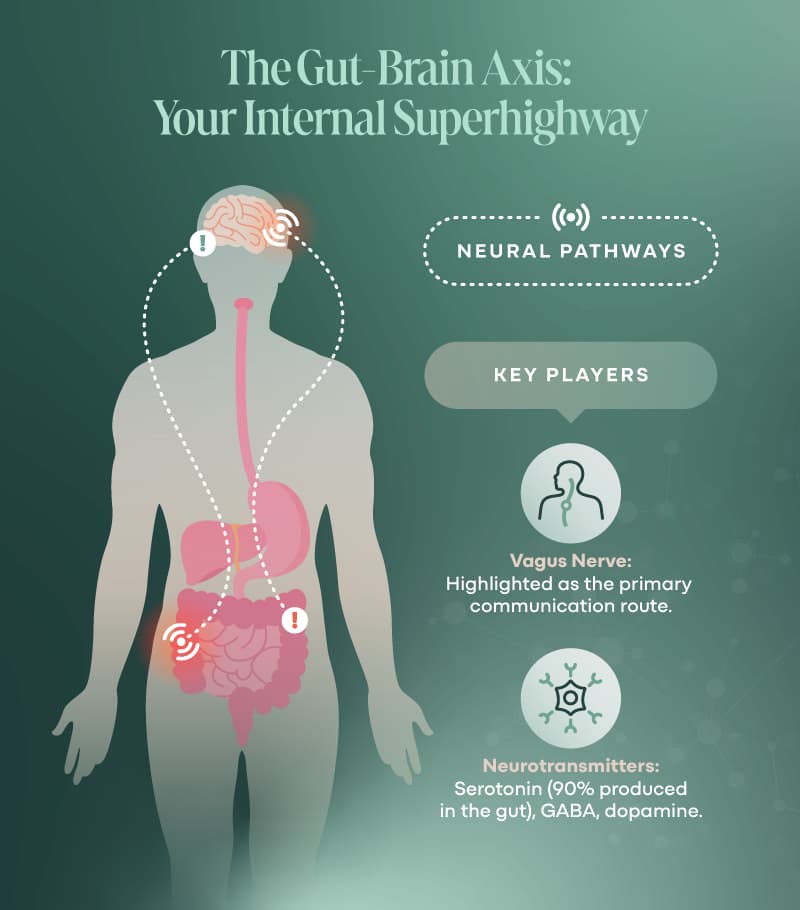
The Gut-Brain Connection: The Vagus Nerve Superhighway
Your gut and brain are in constant conversation (4, 18, 25).
Not occasionally.
Constantly. Like roommates sharing a cramped studio apartment—what affects one, affects the other.
This connection is called the gut-brain axis (2, 4, 15, 16, 17, 18, 25).
It’s a literal communication network made up of nerves, hormones, immune signals, and microbial messengers (2, 4, 18, 25).
The star of the show is the Vagus nerve—a massive, bi-directional cable that runs from your brainstem to your gut, carrying messages both ways (2, 4, 12, 16, 18, 25).
When your gut is inflamed, leaking, or imbalanced, it sends out distress signals through the Vagus nerve—kind of like an overprotective parent calling the school every hour (4, 10, 18).
And your brain responds with anxiety, panic, brain fog, irritability, and disrupted sleep.

You also have a second nervous system inside your gut—the enteric nervous system (4).
It’s so complex it can operate independently of your brain.
It also makes most of your serotonin (yes, the “happy” neurotransmitter), along with GABA (your calming chemical) and dopamine (your motivation mojo) (4, 20, 25).
Which means if your gut bugs are out of whack, so is your mood (9, 13, 24, 25).
That “gut feeling” when something’s off isn’t woo. It’s biology.
Clinical studies have shown strong links between gut disorders like IBS and SIBO and increased anxiety (4, 8, 13, 17, 25).
But you don’t need an official diagnosis to know something’s wrong.
If your digestion’s off, your mind will be too because the gut isn’t just where you digest food.
It’s where you process safety.
And if your gut feels unsafe, you will, too.
The Inflammatory Cascade: How Gut Dysfunction Triggers Anxiety
If you’ve been told your anxiety is “just stress,” I want to gently (but firmly) call BS.
Because for so many, anxiety is a symptom of inflammation—and that fire often starts in the gut (8, 13, 19, 21, 24, 25).
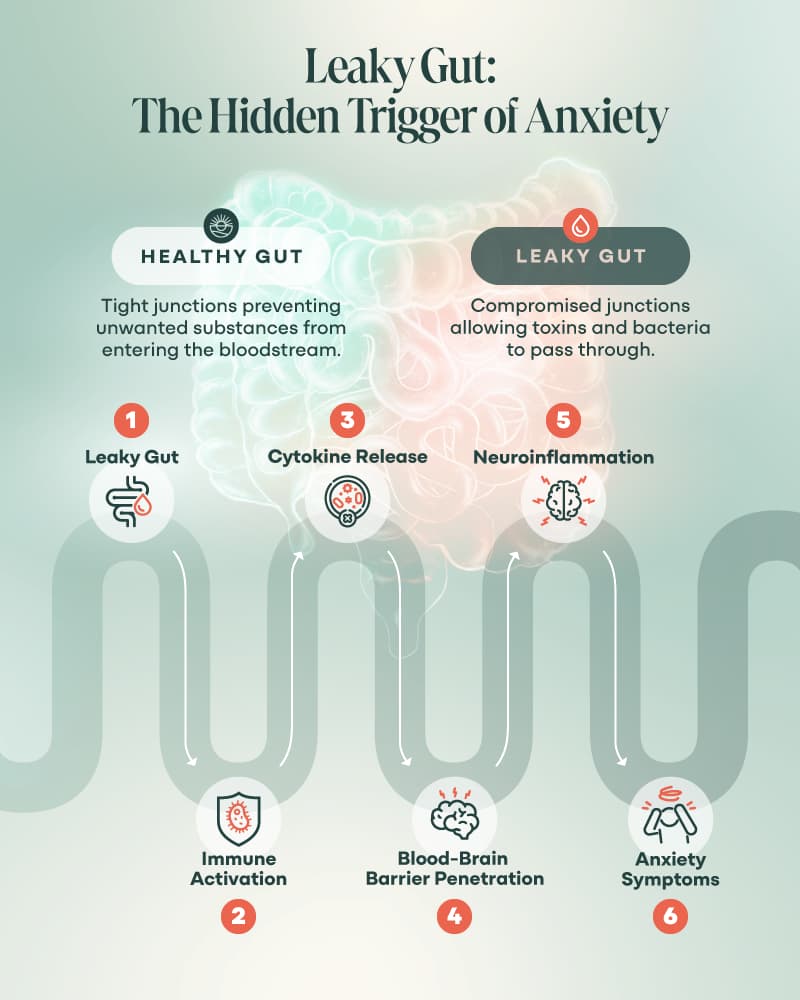
Let’s talk about leaky gut. (Sounds gross, I know.)
When your gut lining gets damaged—by mold, parasites, pesticides, antibiotics, stress, you name it—it’s like poking holes in a coffee filter.
Things that should stay inside your gut (like partially digested food, toxins, and bacterial fragments) leak into your bloodstream (4, 8, 17).
Your immune system sees these as invaders and freaks out, launching inflammatory cytokines to fight back.
Problem is that those cytokines don’t stay put.
They can cross the blood-brain barrier—that protective lining around your brain—and trigger neuroinflammation (4, 8, 17).
How We Can Help
Guiding people to reclaim their health and vitality is our greatest joy. Our entire practice is dedicated to supporting you to be who you really are, at home in your body, because your body is able to heal itself.
Book a CallNeuroinflammation: Gut-Brain Communication
Neuroinflammation is the brain on fire (metaphorically). It’s driven by:
- Cytokines leaking from the gut.
- Cross-activation of microglia, your brain’s immune cells.
- Loss of regulation from the Vagus nerve due to gut stress.
When neuroinflammation is present, your limbic system (fear center) gets hypersensitive (4, 8, 17).
That means more reactivity, more catastrophizing, and a general sense of “I’m not safe.”
You’ll feel wired, restless, irritable, panicky, foggy—sometimes all at once.
This isn’t random. It’s your biology doing its best with a messed-up input system.
Now add in oxidative stress—the byproduct of poor gut health, low antioxidants, and overwhelmed mitochondria.

Oxidative Stress: The Rust That Never Rests
When your gut microbiome is off, you produce more reactive oxygen species (ROS)—essentially metabolic exhaust fumes.
Normally, your antioxidants (like glutathione) neutralize them.
But if you’re depleted (which most chronically symptomatic folks are), ROS run wild.
- This damages the gut lining → leaky gut.
- It crosses the BBB (blood-brain barrier) → neuroinflammation.
- It messes with mitochondrial energy output → brain fog and fatigue. (Hello, mitochondrial dysfunction.)
You feel anxious because your brain is literally under chemical siege (11).
You’re left with a tired, toxic brain that still won’t let you sleep.
And no, meditation won’t fix that.
Not if your gut is sending daily alarm bells to your nervous system.
Chronic inflammation rewires your stress response.
It makes your brain believe you’re in danger all the time.
If you feel like you’re constantly reacting, spiraling, or overthinking everything—there’s a good chance your gut is literally inflaming your thoughts.
Let’s stop pathologizing your anxiety. Let’s start understanding its sources.

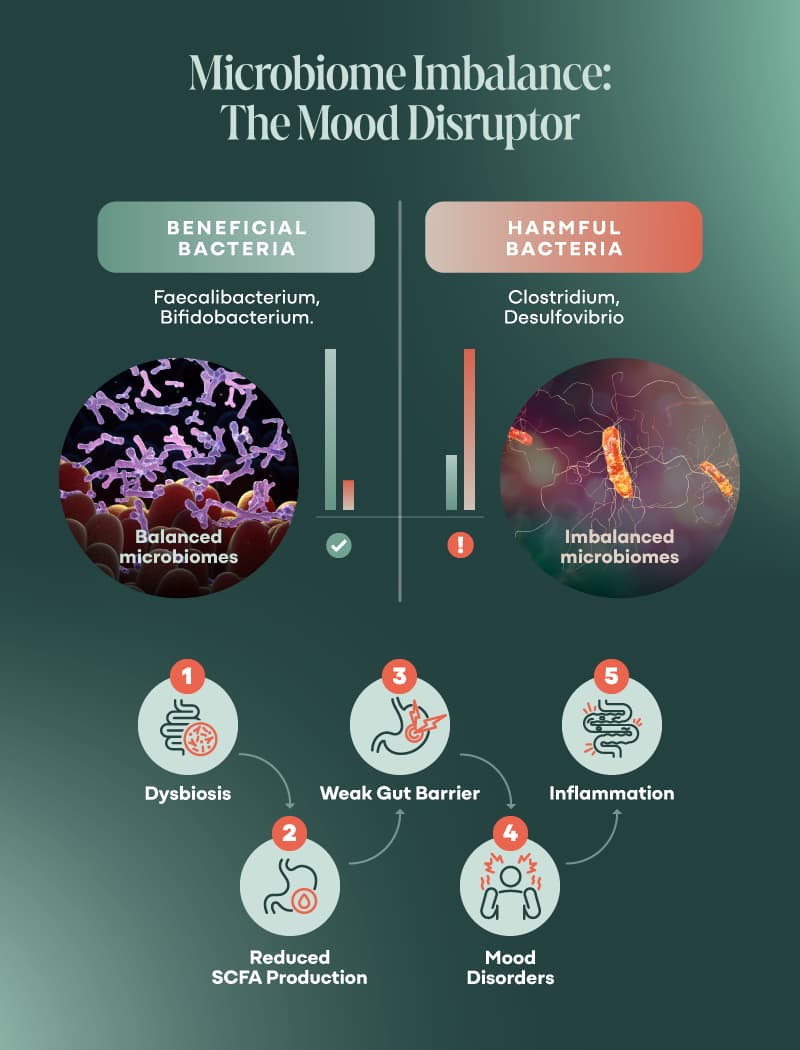
Gut Microbiome: Dysbiosis and Short-Chain Fatty Acids
Dysbiosis is when your gut turns into a bad neighborhood—too many troublemaker microbes, not enough peacekeepers.
It’s what happens when antibiotics, stress, pesticides, parasites, metals, or mold exposure wipes out your microbial diversity, and suddenly the bugs that should be helping you are outnumbered.
Inflammation rises, digestion tanks, and your brain gets the fallout—because when your gut’s out of balance, your whole system is running on the wrong software.
Common troublemakers:
- Bacteroides (16, 24)
- Paraprevotella (16)
- Fusobacteria (3, 24)
- Ruminococcus gnavus (3)
Common peacekeepers:
- Firmicutes (20, 24)
- Akkermansia (20)
- Faecalibacterium (3, 23)

(SCFAs): Nature’s Anti-Anxiety Agents
Let’s talk about something deeply unsexy that’s important to mental health: fiber fermentation.
When you feed your gut microbes fiber—especially from plants—they go to work breaking it down into powerful compounds called short-chain fatty acids (SCFAs), like butyrate, acetate, and propionate (18, 25).
These are chemical messengers that keep the peace across your gut-brain axis.
Butyrate, in particular, is a rock star here (8, 18, 25):
- It strengthens the gut lining, preventing leaky gut.
- It reduces systemic inflammation, including in the brain.
- It increases BDNF (Brain-Derived Neurotrophic Factor)—which helps your brain grow, adapt, and stay mentally resilient. Low levels can lead to anxiety (25).
Low SCFA levels have been linked to higher levels of anxiety and depression (7, 24, 25).
In an animal study, mice deprived of SCFA-producing bacteria developed anxious behaviors—and when those bacteria were reintroduced, the behaviors improved. (No cheese platters or therapy needed.) (7)
If your microbiome is depleted (hello, antibiotics, pesticides, mold, stress), you’re probably not making enough SCFAs.
If you’ve been low-carb for too long, or avoiding veggies because of gut symptoms, you’re starving your internal peacekeepers.
Without SCFAs, the gut lining weakens, inflammation rises, and the brain gets noisy.
You don’t need to micromanage your gut—just feed it like the living ecosystem it is.
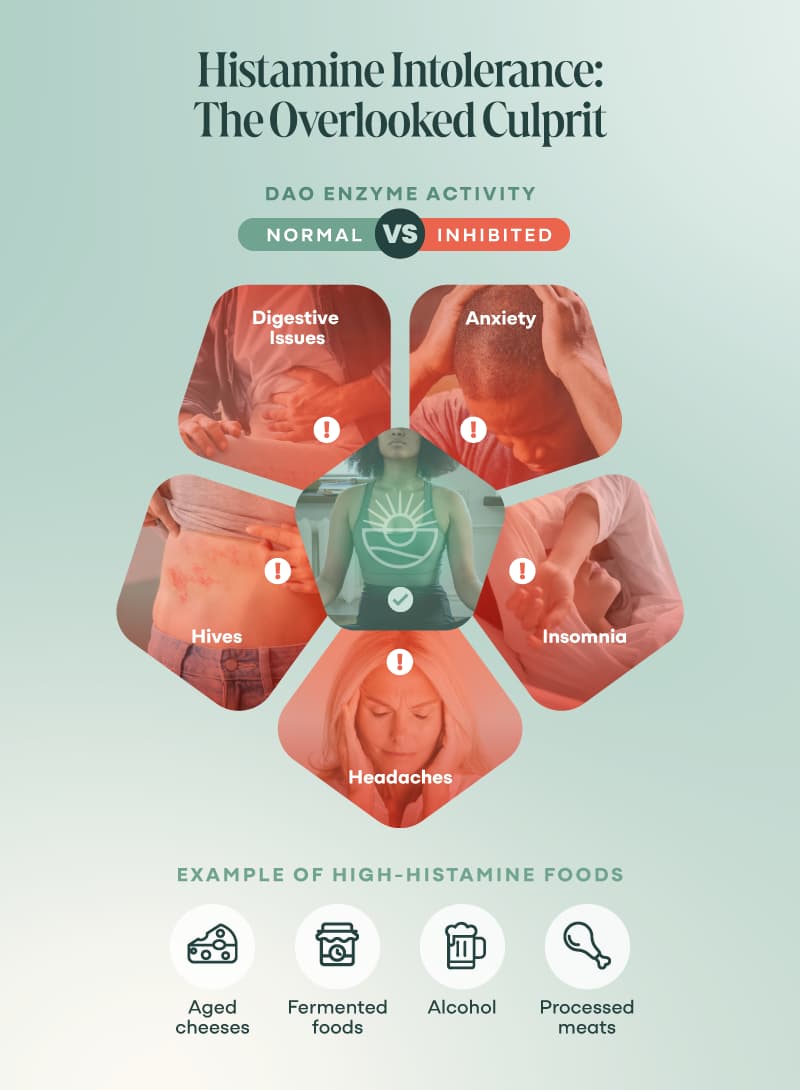
Histamine Intolerance: The Hidden Driver of Panic and Insomnia
Ever felt jittery after a “healthy” meal?
Or wired at bedtime despite being exhausted?
That could be histamine talking—and not in a flirty way.
You probably know histamine as the molecule behind allergic reactions, but it’s also a neurotransmitter that affects alertness, focus, and yes—anxiety.
A little is helpful. Too much? Welcome to the overthinking Olympics.
Your body is constantly producing histamine, and your gut plays a major role in breaking it down using an enzyme called DAO (diamine oxidase).
But if your gut lining is inflamed or damaged, DAO production drops.
Histamine builds up.
And suddenly, your “random” symptoms start making a lot more sense:
- Racing heart or anxiety after meals
- Brain fog or irritability
- Flushed skin, headaches, or hives
- Insomnia despite being bone-tired
What’s sneakier? Certain gut bacteria like Klebsiella and Morganella make histamine (26).
And if you’re dealing with dysbiosis, parasites, or mold toxicity, your gut can become a histamine factory with no off-switch.
High-histamine foods (fermented foods, spinach, avocado, wine, aged cheese) can tip you over the edge, but the real issue is internal overload—not your love of sauerkraut.
So no, you’re not “too sensitive.” You’re biochemically overwhelmed.

Microbial Metabolites and Mental Health: What Is 4-EPS?
If you’ve never heard of 4-EPS (4-ethylphenylsulfate), that’s not your fault—most practitioners don’t talk about it.
But your microbes sure do.
4-EPS is a gut-derived metabolite made by certain bacteria (including some Clostridia species) when they ferment dietary proteins, especially tyrosine.
And when this compound builds up in the bloodstream, it hijacks your neurobiology.
In a now-famous study from Caltech, scientists injected 4-EPS into mice—and what happened next wasn’t subtle (18):
The mice developed extreme anxiety behaviors, avoiding open spaces and freezing in fear.
Later, elevated 4-EPS levels were found in children with autism spectrum disorders and anxiety symptoms.
Translation: this microbial byproduct can seriously disrupt brain chemistry and behavior.
So, what controls 4-EPS levels?
Your gut terrain.
A balanced microbiome keeps these troublemakers in check.
But when the good guys are outnumbered—because of antibiotics, poor diet, parasites, or mold exposure—4-EPS can skyrocket.
This isn’t about demonizing bacteria—it’s about understanding that your microbes are chemical factories, and their outputs affect your brain (18).
You are not a passive host in this equation.
Lowering 4-EPS means rebalancing your gut ecology, restoring integrity to your intestinal wall, and yes—sometimes killing off the chaos (strategically, not randomly).
In addition to altering levels of histamine, SCFA’s, and neurotransmitters, your gut health influences your nervous system directly.
Impact of the Gut on the Nervous System: Why a Dysregulated Gut Dysregulates You
If you feel like you’re living in a constant state of “something’s wrong,” it may be your nervous system— commandeered by your gut (4, 9, 15, 20, 21, 23, 25).
When the gut is inflamed, full of pathogens, or leaking toxins into the bloodstream, your Vagus nerve—that gut-brain hotline—starts screaming like a toddler after skipping naptime.
And instead of sending messages of calm, safety, and digestion, it’s yelling “Code Red!”
Constantly.
That’s how you end up stuck in sympathetic dominance—your body’s “fight, flight, freeze, or fawn” setting.
What does that feel like?
- Restlessness or hypervigilance
- Shallow breathing or chest tightness
- Trouble sleeping, relaxing, or even digesting food
Your brain interprets these physical sensations as anxiety, because it’s trying to make sense of the chaos.
You feel emotionally unstable, reactive, or overwhelmed—not because you’re broken, but because your gut is throwing off your neurological rhythm.
You can’t fully heal your gut if your nervous system is still on high alert.
Detox can become a trauma trigger under these circumstances.
Digestion shuts down. Inflammation rises
Regulation isn’t a luxury—it’s the foundation. Start with:
- Gentle Vagus nerve stimulation (humming, gargling, cold exposure)
- Breathwork and somatic tools
- Nervous system-safe detox strategies
When your gut is safe, your brain can finally relax.

Nutrient Malabsorption: Why You Can’t Supplement Your Way Out
Let’s talk about your supplement graveyard—that collection of half-used bottles you hoped would finally fix your anxiety, fatigue, or brain fog.
And yet… here you are.
The problem isn’t your willpower. It’s absorption.
When your gut is inflamed or imbalanced, your ability to absorb nutrients tanks.
Doesn’t matter how “bioavailable” your magnesium glycinate is—if your gut lining is compromised, it’s like pouring gold into a sieve.
Here’s what gets affected first (27).
- Magnesium – crucial for calming the nervous system
- B vitamins – key for neurotransmitter production and stress resilience
- Zinc – essential for GABA synthesis and gut repair
- Iron – low levels lead to fatigue and anxiety, especially in women
When your gut is a mess, you’re not absorbing them well, no matter how clean your diet is.
Low on these nutrients?
Expect irritability, anxiety, sleep issues, and a fuse the length of a gnat’s eyebrow.
You cannot supplement your way out of gut dysfunction.
It’s like trying to paint a house with a collapsed foundation.
Before you invest in another nootropic or adaptogen stack, ask: “Is my gut even capable of using this right now?”
Real healing means:
- Calming the nervous system
- Rebuilding terrain and establishing flow
- Removing blocks (inflammation, pathogens)
- Reintroducing nutrients when the body can actually use them
Otherwise, you’re just making expensive pee.

Take Care of Your Gut Health to Ease Anxiety
You might be thinking, “Okay, I get it—my gut’s a mess. But where do I even start?”
The healing path isn’t about doing everything at once. It’s about doing the right next thing.
Step 1: Calm the nervous system daily
Vagus nerve support isn’t optional.
Breathwork, grounding, safe movement, and trauma-informed nervous system tools all make your gut more responsive to healing.
Step 2: Stop feeding the chaos
Cut back on inflammatory triggers: ultra-processed foods, refined sugar, seed oils, alcohol, and chronic stress.
Yep, stress feeds bad bugs too. (Parasites love a late-night doomscroll.)
Step 3: Open the drainage pathways
Before you kill anything off or detox, make sure your body can get rid of waste.
Drainage means pooping daily, sweating regularly, lymph movement, and bile flow.
Otherwise, you’re just moving toxins around and calling it healing.
Step 4: Support your mitochondria
Your brain is a power-hungry organ, and your mitochondria—those tiny energy factories inside your cells—are what keep it running.
But when your gut is inflamed or toxic, mitochondrial function tanks, leaving you foggy, fatigued, and way more prone to anxiety.
Supporting your mitochondria with targeted nutrients (like CoQ10, PQQ, and B vitamins) and reducing oxidative stress helps restore mental clarity, energy, and emotional resilience—right from the cellular level.
Step 5: Address Root Causes
Once the basics are covered, and your body is in a safe position to heal, now you can tackle the underlying root causes of your gut dysfunction.
- Mold? Eliminate mold sources from your environment and your body.
- Parasites? Make yourself a poor host and evict those annoying freeloaders!
- Toxins? Reduce exposures and detox them from your body.
- Metals? Escort them out with binders.
- EMFs? Rebalance your biofield and cellular energy to heal your electrical body.
The synergy between root causes can make even small amounts of exposure a big deal.
Working with a seasoned practitioner is imperative so you resolve your root causes in the right order and at a pace your body can handle.
This isn’t about perfection. It’s about progress and alignment.
This Is Your Body Calling You Back to Yourself
Gut dysfunction doesn’t just correlate with anxiety—it drives it.
From SCFA deficiencies to 4-EPS toxicity, your mental health is responding to the chemistry of your internal terrain.
If you’ve been blaming yourself for your anxiety, I want you to hear this loud and clear:
Your body is not broken—it’s communicating.
That racing mind? The sleepless nights? The undercurrent of panic for no apparent reason?
They’re often biochemical distress signals from your gut.
And the good news is that these signals are reversible.
When you start clearing toxic inputs, restoring gut integrity, and regulating your nervous system, anxiety doesn’t have to be your default anymore.
Because when you heal your gut terrain, you quiet the internal alarm bells.
You stop spiraling. You sleep deeper. You breathe easier. You come back to yourself.
That’s the real you. The resilient one. The one who’s not ruled by fear—but by flow.
How We Can Help
Guiding people to reclaim their health and vitality is our greatest joy. Our entire practice is dedicated to supporting you to be who you really are, at home in your body, because your body is able to heal itself.
Book a CallFAQs
Can gut microbes and issues really cause anxiety?
Yes. Inflammation, dysbiosis, and intestinal permeability send distress signals to your brain, triggering anxiety—even without external stress.
What if I’ve already tried probiotics and they didn’t help?
That’s common. If your terrain is inflamed or your drainage pathways are blocked, probiotics won’t stick. Terrain first, then bugs.
Is this just about food sensitivities?
Nope. It’s about why your body is reacting—think: histamine buildup, intestinal permeability, or microbial toxins, not just the spinach.
I don’t have digestive symptoms. Could this still be my gut?
Yes. Anxiety, fatigue, insomnia, and brain fog are all gut-related—especially when inflammation travels silently.
What’s the fastest way to start calming my gut-brain axis (or brain-gut axis)?
Start with nervous system regulation. If you’re not in a healing state, nothing else will stick.
Will this help with panic attacks or just general anxiety?
Yes—by calming the underlying biological chaos, you lower the volume on both chronic and acute anxiety patterns.