Mast Cell Activation Syndrome (MCAS) is a chronic immune disorder in which mast cells overreact, triggering widespread symptoms without a clear allergen. Learn how this misunderstood syndrome affects your entire body.
You walk into a store and catch a whiff of perfume.
Within seconds, your heart’s racing, your face flushes, and your head fills with that weird underwater pressure again.
You can’t think.
You can’t breathe.
You leave your cart in the aisle and bolt for the door. Again.
You’ve cleaned up your diet. You’ve tried the protocols. And still, your body seems to be reacting to everything, even your own sweat.
It’s like your immune system is in a permanent state of “freak out,” and no one can tell you why.
Your body is reacting like it’s under siege—because in a way, it is.
Enter: Mast Cell Activation Syndrome, or MCAS.
MCAS isn’t just an allergy thing, and it’s not a “sensitive person” thing. It’s a real, under-identified condition where your immune system’s frontline soldiers—your mast cells—start misfiring.
Constantly. To things that shouldn’t be a threat.
Think of them like those old-school car alarms that go off when a butterfly lands on the hood.
In this article, we’re going to take a closer look at MCAS and—most importantly—how to start helping your body calm the heck down.
Key Takeaways
- Mast cells are complex, powerful, and everywhere.
- MCAS is a real, underdiagnosed immune disorder—Not “just allergies.”
- Healing requires a whole-body, gentle approach.

What Are Mast Cells, and Why Do They Hate Me?
Let’s clear something up right away: mast cells are not your enemy.
I know, they feel like it when your face randomly swells up after eating avocado, or you get hives from sunlight.
But these cells aren’t sabotaging you—they’re trying to save you. They’ve just gone a little, well, rogue.
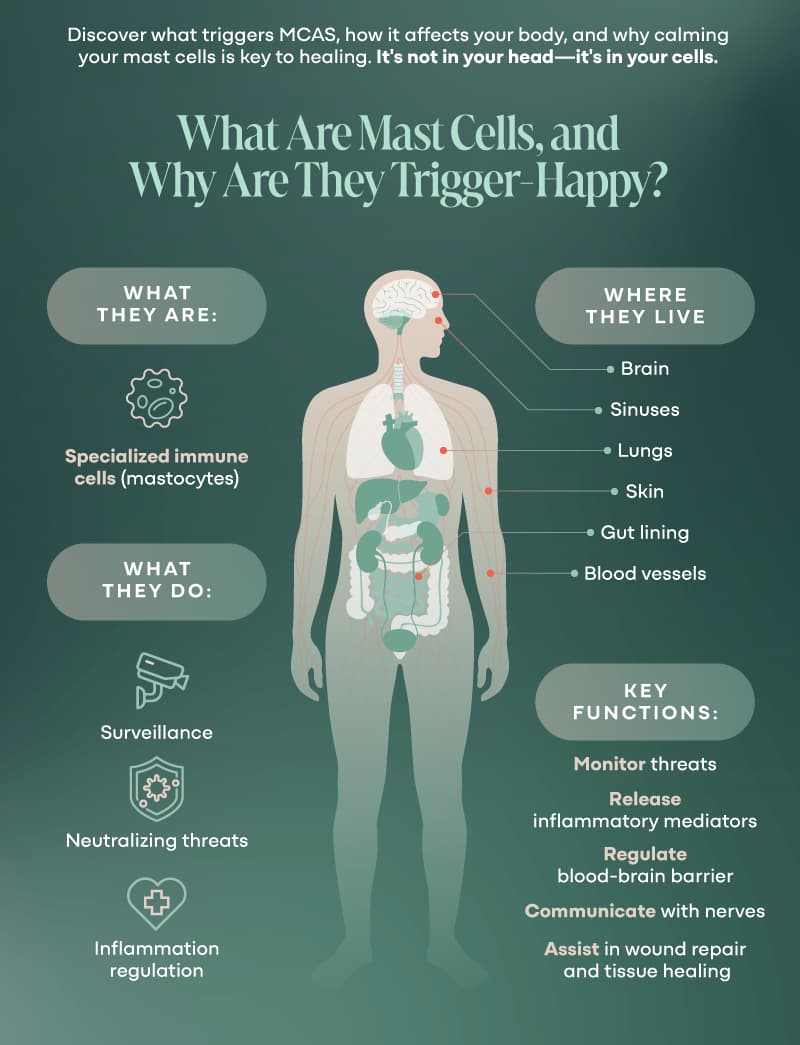
Mast cells (aka mastocytes) are a type of white blood cell, and they’re nothing short of miraculous when they’re doing their job well.
Their job is to detect threats, regulate responses, neutralize invaders, and keep the peace (16, 17, 23, 24).
Unlike most immune cells that float around in your blood, mastocytes live full-time in your tissues—especially the areas most exposed to the outside world (4, 10, 11, 16, 17, 22, 23, 24):
- Your skin
- Your gut lining
- Your lungs
- Your sinuses
- Your brain (yep, they hang out there too)
Why?
Because they’re strategic.
These cells park themselves right where trouble is most likely to show up.
Interesting Mast Cell Facts
The literature is filled with interesting info about mastocytes. I picked several fascinating tidbits to share with you:
- They extend a portion of themselves through microscopic gaps in blood vessel walls so they can surveil your blood to detect circulating IgEs and capture enemy molecules (23)!
- The release of substances from mastocytes (collectively called Mast Cell Mediators) is regulated by a circadian clock (23)
- An overreactive mastocyte is called “unstable.” They can retain a “memory” of past triggers to respond more rapidly to the same or similar triggers in the future. Past stress can “prime” your mastocytes to respond more aggressively to future stress (23).
- They regulate blood-brain-barrier permeability and are the “immune gate to the brain” (23).
- Mastocytes can be activated by direct binding to the SARS-CoV-2 virus (11).
- Mastocytes can sense the release of neurotensin and Substance P and thus interact directly with sympathetic nerves (11, 23).
- They can store preformed molecules or make what they need in the moment. They can release these molecules all at once (anaphylaxis), or a little bit at a time (10, 13, 17, 22, 23, 24).
- Each mastocyte can store or synthesize several hundred different chemicals (10, 13, 24).
- Yeast stimulates mastocyte to secrete pro-inflammatory chemicals (23)
- They provide the link between innate and acquired immunity, participate in antigen presentation, and promote tissue repair (2).
- Cellular energy (ATP) located outside of the cell can activate mastocytes (17).
Mast Cell Danger Response
When mastocytes sense danger, they release a chemical cocktail of inflammatory mediators—including histamine, cytokines, prostaglandins, and tryptase (2, 13, 16, 17).
These substances increase blood flow, recruit other immune cells, and help your body mount a defense.
But in MCAS, those cells are no longer just responding to real threats.
They’re reacting to everything—foods, stress, heat, smells, EMFs, your favorite lotion.
And because mastocytes don’t just live in one spot, the symptoms can show up anywhere: skin, gut, heart, brain, bladder.
This is why MCAS is often mis-identified as a dozen different conditions—or just dismissed entirely.
When mastocytes are overreacting, it’s a signal that something in your internal terrain is pushing them into overdrive.
Maybe it’s unresolved infections.
Maybe it’s toxic overload.
Maybe it’s unresolved trauma stored in your tissues.
Usually? It’s a little bit of all the above. That’s why we don’t just suppress mastocytes with meds and hope for the best.

Histamine and Other Mast Cell Mediators
Let’s talk about histamine—the misunderstood middle child of your immune system.
If you’ve got MCAS, someone’s probably told you to avoid high-histamine foods.
But histamine isn’t evil. It’s essential.
Histamine helps you:
- Fight infections (8, 17)
- Regulate stomach acid (so you can digest food and absorb nutrients) (8, 17)
- Constrict and dilate blood vessels (hello circulation) (7)
- Signal between neurons (meaning: it’s crucial for brain function) (8, 17)
- Wake up in the morning (your brain releases histamine to get you out of bed) (7, 9)
- Manage stress (facilitates the release of stress-related hormones and neurotransmitters) (9)
It’s kind of the Swiss Army knife of your body’s communication system.
But like any multitasker, when it’s overworked and unregulated, it causes chaos.
Think headaches, skin flushing, bloating, insomnia, anxiety, and that classic histamine hangover: brain fog, fatigue, and irritability.
Where Does Histamine Come From?
Histamine is mostly produced in your mastocytes, but not just them. Other sources include:
- Basophils (another type of immune cell)
- Neurons (especially in your brain’s “wake-up” center)
- Certain gut bacteria (yes, some microbes make histamine) (8)
- Food (especially aged, fermented, smoked, or leftovers that sat a little too long) (1, 8)
This means you can have high histamine levels even if your mastocytes are behaving—though in MCAS, they usually aren’t.

How Does Histamine Cause Signs and Symptoms?
Histamine causes symptoms through receptors—tiny docking stations on your cells that respond to different “flavors” of histamine signaling (2, 7, 9).
Each receptor creates a different kind of chaos when overstimulated:
- H1 receptors: itchy skin, rashes, hives, sneezing, headaches, anxiety, insomnia, asthma, anaphylaxis (7)
- H2 receptors: stomach acid, heartburn, immune modulation, sometimes dizziness(7)
- H3 receptors: mostly in the brain—regulate neurotransmitters and affect cognition, sleep issues, ADHD, obesity, and cognitive disorders (7, 9)
- H4 receptors: influence immune cells and inflammation in organs like the gut, lungs, pancreas, liver, and bile ducts (7)
This is why a single antihistamine rarely fixes the problem—it only blocks one receptor type (1). It’s like trying to stop a flood with a single sandbag.
And remember, histamine is just one of over 200 mediators released by mastocytes.
Lucky you—you can have mastocytes in various parts of your body releasing different combinations of mediators at the same time (13)!
So, if you’ve ever felt like your symptoms are all over the map—heart racing one day, hives the next, followed by diarrhea and total brain shutdown—it’s not in your head.
It’s in your mast cells.
And their chemical tantrums are loud, varied, and exhausting.
Now that we understand histamine basics, let’s look at the various mast cell disorders.

Types of Mast Cell Disorders
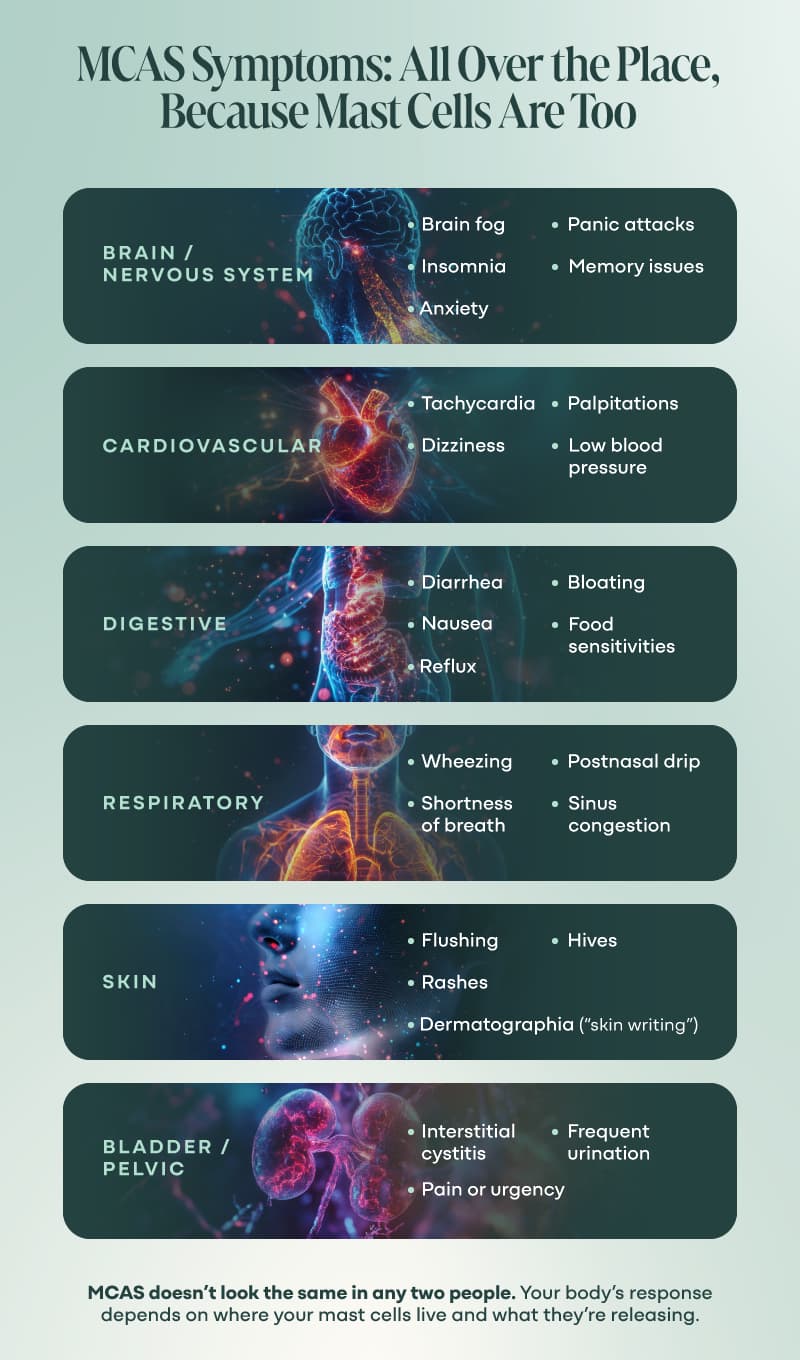
Mastocyte disorders can present with a wide variety of symptoms: itching, flushing, shortness of breath, rapid, heart rate, diarrhea, nausea, vomiting, reflux, GI discomfort, headache, fatigue, rash, hives, dermatographia (aka “skin writing”), acid reflux, blood pressure instability, angioedema, interstitial cystitis, pain or urgency with urination, palpitations, dizziness, wheezing, pain, depression, irritability, brain fog, and memory loss (4, 12, 13, 14, 16, 18, 23, 25).
These symptoms often mimic other conditions like GERD, IBS, menopause, anxiety, and food intolerances.
Let’s review the spectrum of mast cell disorders, so you can understand where MCAS falls.

Primary Mast Cell Disorders (Clonal)
These involve abnormal cloning of mastocytes, usually with a genetic mutation (5, 14, 15, 16,17, 22).
- Systemic Mastocytosis (SM): Involves at least one extra-cutaneous organ, typically bone marrow. Identified via WHO criteria based on tissue biopsy, serum tryptase, and KIT mutation (23, 24).
- Cutaneous Mastocytosis (CM): Affects the skin, especially in children, and typically resolves by puberty (23).
- Monoclonal Mast Cell Activation Disorder (MMCAD): Occurs in patients with anaphylaxis or Hymenoptera venom sensitivity. Clonal mastocytes may be found, but without meeting full criteria for SM (23).
Secondary Mast Cell Disorders (Reactive)
Normal mastocytes reacting to known triggers (5, 14, 15, 16, 17, 22).
- IgE-Mediated Hypersensitivity: Classic allergic reaction to things like foods, insect venom, and pollens. Triggered by allergen-bound IgE (23).
- Non-IgE-Mediated / Drug-Induced Activation: Drugs (e.g., NSAIDs, opioids, muscle relaxants) trigger mastocytes via MRGPRX2 receptor (23).
- Mast Cell Hyperplasia: Increased mastocytes due to autoimmune diseases, infections, and cancers (23).
Idiopathic Mast Cell Activation Syndrome (MCAS)
This is what we’re talking about! Mast cell activation without a detectable trigger or cell cloning abnormality (2, 5, 10, 12, 14, 15, 16, 17, 22).
These are the most common category of mast cell disorders (5, 10, 23).
- Patients have typical symptoms (e.g., flushing, GI upset, hypotension, brain fog), normal mast cell counts, and no KIT mutations (14).
- Symptoms are episodic, multisystemic, and often triggered by stress, infections, or unknown stimuli (2, 11, 23, 24).
- Often called non-clonal MCAS, idiopathic MCAS, or mast cell mediator disorder (10, 23).
To complicate the issue, Hereditary Alpha-Tryptasemia (HaT) is a genetic trait that leads to elevated baseline tryptase levels (15).
It can mimic MCAS symptoms or modify severity in true MCAS cases (15).
What Makes MCAS So Sneaky?
With MCAS, your mastocytes aren’t increasing in number—they’re just way too reactive (2, 25).
They keep misfiring, releasing histamine and other inflammatory mediators at the drop of a hat—or a whiff of perfume. Or a bite of avocado. Or a change in temperature. Or stress. Or nothing at all.
Your body’s security system is stuck on high alert, and everything looks like a threat.
Here’s the challenge:
MCAS doesn’t look the same in any two people.
You might get hives and a racing heart.
Someone else might get migraines and diarrhea.
Another person might just feel exhausted and mentally scrambled 24/7.
The symptoms you have will be determined by which of the 200+ chemical mediators are released (16, 24). For example:
- Histamine: Itching, headaches, and low blood pressure (23); smooth muscle contraction (2)
- Tryptase: Inflammation, clotting issues (2)
- Cytokines: fatigue and inflammation (23), increased mucus production (2)
- Leukotrienes: Bronchoconstriction, wheezing (2, 23)
- Heparin: Blood thinning (2)
And because mastocytes live in pretty much every tissue in your body, they can cause symptoms in (you guessed it) pretty much every system.
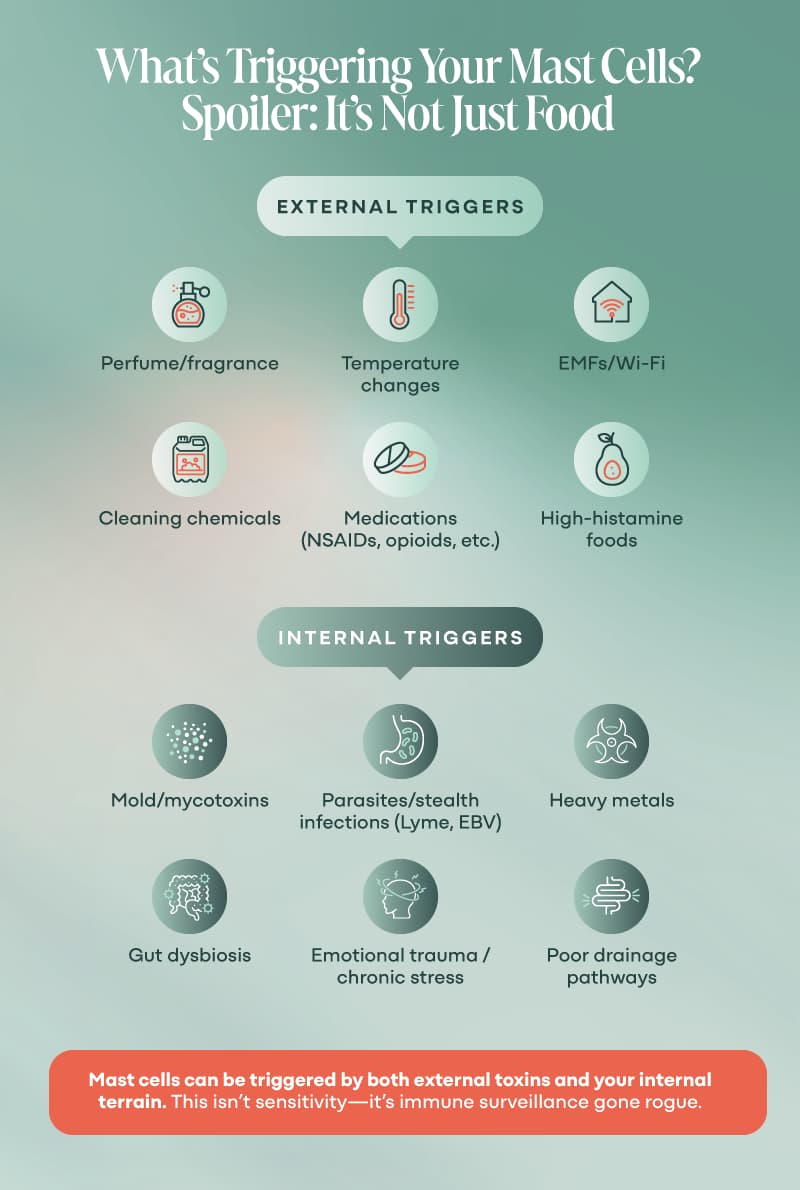
Mast Cell Activation and Triggers
Triggers can vary wildly, but here are some of the big ones:
- Mold exposure (especially mycotoxins) (4, 22, 23)
- Heavy metals (like mercury or aluminum) (22, 23)
- Parasites and stealth infections (hello, Lyme, EBV, Bartonella, yeast) (22, 23)
- Pesticides and chemical sensitivity (22, 23)
- EMFs and Wi-Fi overload (yes, researchers are starting to look at this) (22)
- Food sensitivities (not allergies—those are IgE. This is different.) (23)
- Stress and trauma (emotional stress can literally degranulate mastocytes) (22, 23)
Your mastocytes are paying attention to your external environment—but they’re also deeply affected by your internal terrain: gut dysbiosis, mitochondrial dysfunction, poor drainage, past infections, stored trauma, and more.
If your system is loaded down with toxic burden or stuck in fight-or-flight, mastocytes pick up on that and go full red alert.
The frustrating part?
You often don’t know it’s MCAS.
“Oh, flushing and insomnia and bloating and heart palpitations? Must be your mast cells.” Said no one, ever.
You get bounced between dermatologists, GI specialists, cardiologists, allergists, and therapists—each one treating a different “symptom set” instead of seeing the whole picture.
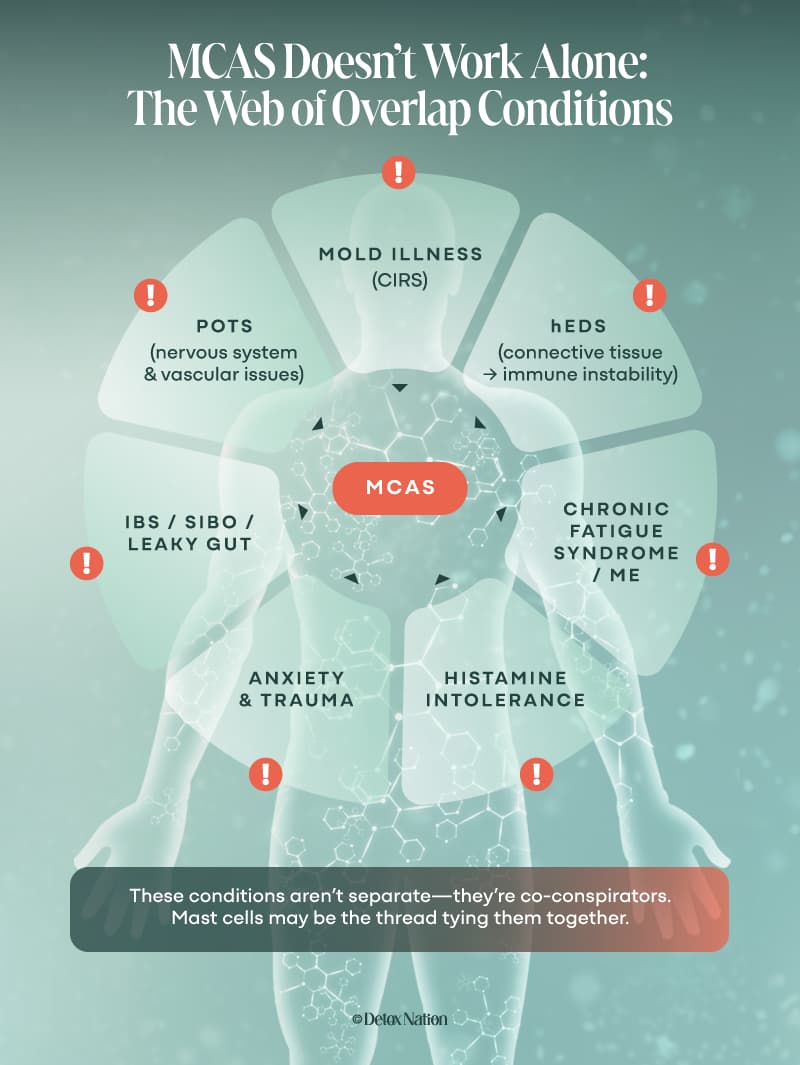
Co-Conspirators: Conditions Often Found with MCAS
MCAS is rarely a solo act.
If you have MCAS, chances are high that you’ve also got at least one of its close cousins riding shotgun.
Maybe you’ve been diagnosed with them. Maybe not.
But understanding these co-morbidities can help you stop chasing your tail—and start untangling the web.
Let’s meet the usual suspects:
POTS (Postural Orthostatic Tachycardia Syndrome)
Ever stand up too fast and feel like you’re going to pass out? Or like your heart’s trying to escape your chest? That’s POTS (11, 13, 19). It’s a form of dysautonomia—aka, your nervous system’s broken thermostat.
It’s super common in people with MCAS because mastocytes can wreak havoc on your vascular system and interfere with blood pressure regulation.
Add in poor hydration, electrolyte imbalances, and histamine-induced vasodilation?
Boom—dizzy, shaky, nauseous mess.
hEDS (Hypermobile Ehlers-Danlos Syndrome)
This one’s the bendy body type.
Think: super flexible joints, chronic pain, frequent injuries, stretchy skin.
hEDS is a connective tissue disorder, and while it might seem unrelated (21), there may be a huge overlap with MCAS (6).
Why?
Your connective tissue is full of mast cells.
Plus, when your body structure is compromised, it puts stress on every other system—including your immune and nervous systems.
IBS, SIBO, and Leaky Gut
If your gut is a war zone, MCAS is likely involved.
Mast cells line the GI tract like paranoid bouncers, ready to react.
They can make your gut hyper-permeable (leaky), slow down motility (hello SIBO), and trigger pain, bloating, or diarrhea every time you eat (14).
And don’t be fooled by the label “IBS.”
It’s not a diagnosis—it’s a shrug in four letters.
Chronic Fatigue Syndrome / ME
You might be too exhausted to even question your exhaustion anymore.
MCAS-induced inflammation, mitochondrial dysfunction, and sleep disruption can all contribute to crushing fatigue.
Add in coexisting infections like EBV or Lyme, and your body just can’t recharge.
Anxiety, Panic Attacks, and Trauma
You’re not “just anxious.” Your mastocytes literally release neuroinflammatory substances—like histamine and cytokines—directly into your brain.
So, when you feel panicky “for no reason,” that may be the reason.
Add a dysregulated nervous system to the mix, and now your trauma history and mast cells are in a feedback loop nobody asked for.
Mold Illness (CIRS)
Mast cells don’t like mold. Full stop.
Mycotoxins (the chemical weapons mold releases) are one of the most potent triggers we know of.
If you’re reacting to everything and have symptoms that flare when you’re in certain buildings or climates?
Mold might be behind the curtain—pulling the strings.
Here’s the bottom line: if you’ve been handed five different diagnoses that don’t seem to fit together, MCAS may be the thread that ties them all.
You’re not falling apart. You’re dealing with a whole-system response.
Next, we’ll tackle one of the hardest parts of the MCAS journey: why it takes so long to get identified, and how to keep going when the system keeps telling you “it’s nothing.”

Why Diagnosis Feels Like an Episode of “CSI: Gaslight” (aka Living with Mast Cell Activation Syndrome)
You know the drill by now.
You make the appointment.
You explain your symptoms—again.
You list out the reactions, the weird food triggers, the rashes, the insomnia, the panic that shows up out of nowhere.
Maybe you even bring a symptom tracker or lab printouts, just to prove you’re not making this up.
The provider listens politely, furrows their brow, and says, “Your tests look normal. Maybe it’s stress?”
Cue internal scream.
The truth is, MCAS is notoriously hard to identify.
Not because it’s rare—but because it’s not well taught, not well understood, and frankly, not profitable for the conventional system.
It doesn’t fit neatly in one specialty.
It doesn’t show up clearly on standard labs.
And most providers don’t even know to look for it.
The average time to diagnosis?
Over a decade. That’s ten years of being dismissed, misdiagnosed, or just quietly suffering in isolation.
And let’s talk about that emotional toll for a second.
Living with unexplained symptoms—especially when people around you can’t see them—can fracture your confidence, strain relationships, and trigger legitimate trauma.
You start to question your instincts. You stop talking about your symptoms. You shrink to fit the mold of “normal.”
But here’s the good news: once you know what you’re dealing with, you can stop playing medical whack-a-mole. You can begin to build a real, step-by-step plan to calm your system and feel safe in your body again.
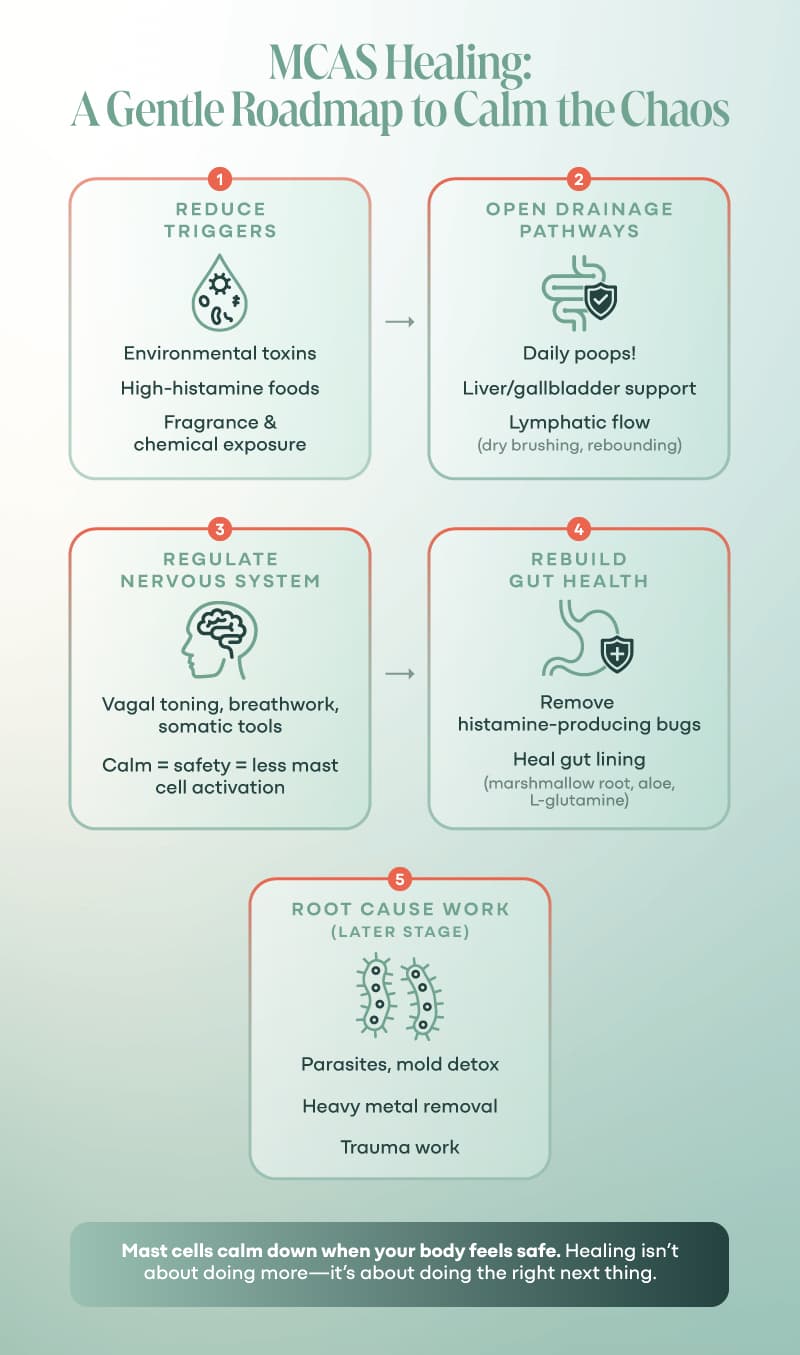
A Gentle, Strategic Approach to Calming Your Mast Cells
If MCAS has taught you anything, it’s this: your body doesn’t respond well to force.
You can’t out-supplement, out-diet, or out-hack your way through a system that’s overwhelmed.
You must work with it. Slowly. Kindly. Intelligently.
Your cells don’t calm down because you demand it—they calm down when your body starts to feel safe again.
And creating that safety isn’t just emotional (though that matters too)—it’s physiological. Biochemical. Electrical. Environmental.
Here’s how you start to rebuild trust with your body when it’s been stuck in a chronic state of defense:
Identify and Reduce the Major Triggers
First, lower the noise. That means removing—or at least reducing—the most obvious stressors:
- Moldy environments
- High-histamine and processed foods (short term, not forever)
- Harsh cleaners and synthetic fragrances
- EMF exposure (especially near the bed)
- Toxic body care and “natural” supplements that are sneakily reactive
You don’t have to be perfect. Just reduce the daily static so your system can breathe.

Support Drainage and Detox—Gently
If your body can’t eliminate toxins, they recirculate—and you’ll keep having symptoms.
Open the exit doors:
- Daily bowel movements (non-negotiable)
- Gentle liver support (think bitters, castor oil packs, not 12-day flushes)
- Lymph movement (dry brushing, rebounding, fascia release)
- Kidney and skin support (hydration, sauna if tolerated, sweating)
This is the foundation. No upstream detoxing until this is in place.
Regulate the Nervous System—Every. Single. Day.
Mastocytes and the nervous system are in constant communication.
If you’re stuck in fight-or-flight, your immune system is too.
- Vagal toning (humming, gargling)
- Somatic practices (even 5 minutes counts)
- Nature time
- Breathwork that calms, not stimulates
- Creating micro-moments of safety in your day
You don’t have to be Zen. Just give your body proof that it’s not in danger anymore.
Rebuild the Gut and Eat a Nourishing Diet
Because if your gut is leaky, inflamed, or full of histamine-producing bugs, your mastocytes will keep reacting.
- Strengthen the gut lining
- Rebalance the microbiome after the terrain is cleaner
- Avoid triggering foods short-term while you heal, but don’t live on five foods forever
- Track symptoms, not just ingredients—what your body’s reacting to can change as you heal
Remove the Root Causes of Your MCAS Symptoms — At the Right Time
Once your system is more stable, you can go deeper.
- Parasite cleansing
- Mold remediation and detox
- Addressing heavy metals, stealth infections, and stored trauma
- Use binders and antimicrobials strategically—not just because TikTok told you to
Healing isn’t about doing more. It’s about doing the right next thing.
Bringing It All Together
As we wrap up, let’s just pause for a second—because you’re still in it.
Still choosing curiosity over collapse.
That’s not a small thing, and it deserves celebration.
MCAS isn’t easy to live with.
It’s invisible, unpredictable, and completely misunderstood by most of the system you’re supposed to trust with your health.
It’s full of gaslighting, guesswork, and grief.
But I want you to hear me: MCAS sucks, and it’s fixable.

FAQs
What is MCAS?
MCAS (Mast Cell Activation Syndrome) is a condition where your mastocytes overreact and release inflammatory chemicals in response to everyday triggers—like foods, smells, temperature changes, or stress—even when there’s no real threat.
How is MCAS different from allergies?
Unlike classic allergies, which are usually IgE-mediated and predictable, MCAS reactions can be unpredictable, widespread, and not tied to a single allergen. It’s immune system chaos, not a simple allergic response.
What triggers MCAS symptoms?
Triggers vary from person to person, but common ones include mold, certain foods, chemicals, infections, stress, trauma, heat, cold, and even EMFs. Often, it’s a combination of internal and external stressors.
What are common MCAS symptoms?
MCAS can affect nearly every system in the body. Symptoms might include hives, flushing, headaches, brain fog, fatigue, gut issues, anxiety, rapid heart rate, and more. They often come in waves and seem disconnected—until you connect the mastocyte dots.
Why is MCAS so hard to diagnose?
There’s no single test for MCAS, and many conventional providers aren’t trained to recognize it. Symptoms can mimic other conditions, and standard labs often miss the root cause.
Can you have MCAS without high histamine levels?
Yes. Histamine is just one of over 200 mediators mastocytes can release. Even if histamine levels are normal, other inflammatory chemicals could still be causing major symptoms.
Can MCAS be treated or healed?
Yes—while there’s no quick fix, MCAS can be managed and often improved dramatically by addressing triggers, supporting detox and drainage, calming the nervous system, and gently restoring balance to the immune system.